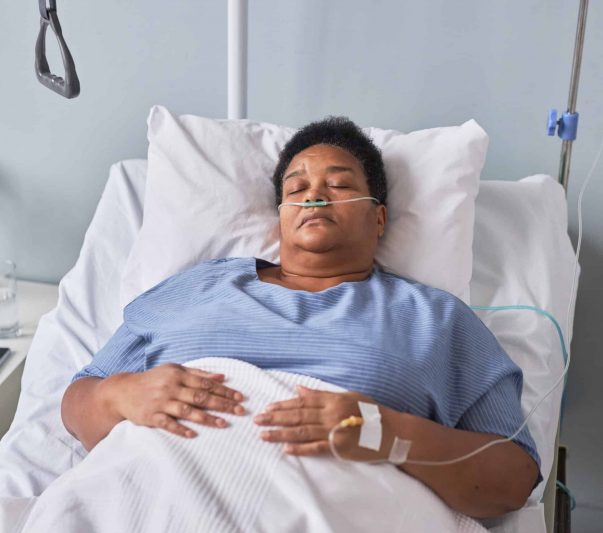
Sepsis is a life-threatening medical emergency that can progress quickly, causing widespread inflammation, organ failure, and, if left untreated, death. It can develop in hospitals, nursing homes, and other care settings. According to the Centers for Disease Control and Prevention, sepsis affects an estimated 1.7 million Americans each year, making it a major public health concern.
Understanding the stages of sepsis can help families and advocates recognize when symptoms were missed, treatment was delayed, or medical care fell below accepted standards. Under the updated Sepsis-3 definition, health care providers classify sepsis based on its progression from initial infection to septic shock, which helps determine urgency and treatment strategies. Recognizing these stages can empower families to speak up when care is inadequate.
If you believe a delayed sepsis diagnosis or poor infection management caused harm to you or a loved one, Olson Personal Injury Lawyers can help.
Key Takeaways
- Sepsis can rapidly progress and may become fatal within hours without prompt treatment.
- Early recognition, rapid antibiotic administration, and effective care coordination are critical to survival.
- Negligence such as missed warning signs, poor documentation, or delayed treatment in hospitals, nursing homes, or rehab facilities may warrant legal action.
How Sepsis Starts and Why Early Action Matters
Sepsis begins with an infection. Something as common as pneumonia, a urinary tract infection, or a skin wound that requires the body to fight an infection can become exacerbated and cause widespread inflammation. This dangerous chain reaction can cause damage to tissues and organs and can quickly shift a simple infection into a life-threatening emergency.
Under the Sepsis-3 consensus definition, sepsis progresses through three main stages:
- Initial Infection: Harmful bacteria, viruses, or fungi invade the body and begin to damage tissues.
- Systemic Inflammatory Response: A heightened, body-wide immune reaction triggered by the infection, causing inflammation.
- Sepsis: The body’s response becomes overwhelming, leading to widespread inflammation and organ dysfunction, which, if left untreated, can cause irreversible damage.
For patients in hospitals or nursing homes, recognizing early warning signs is critical. Families should also be aware of caregiver neglect signs, including delayed medical evaluation, failure to monitor changes in condition, or poor communication between staff members. These lapses can mean the difference between swift treatment and preventable tragedy.
The Current Medical Classification: Updated Sepsis Guidelines
According to the Sepsis-3 consensus and the 2023-2024 WHO guidelines, sepsis is defined as life-threatening organ dysfunction caused by a disregulated host response to infection. Medical professionals typically use the Sequential Organ Failure Assessment, or SOFA, score to measure the extent of organ impairment and track progression.
Sepsis generally advances through three main stages: early sepsis, sepsis with organ dysfunction, and septic shock. The sooner the condition is recognized, the greater the patient’s chance of survival. For families, knowing these stages and their warning signs can be critical.
Stage 1: Early Sepsis - Critical First Signs
Early sepsis occurs when an infection triggers a severe immune reaction that begins to impair organ function. Warning signs include:
- Fever
- Abnormal body temperature
- Rapid heart rate
- Rapid breathing
- Confusion
- Unusual fatigue
This stage has a “golden hour” of recovery, where receiving antibiotics and fluids within the first 60 minutes of recognition can dramatically improve survival.
With prompt treatment, survival rates for early sepsis can exceed 80%, but missed diagnoses are still common. In busy hospital wards or understaffed nursing homes, early sepsis symptoms may be mistaken for less serious illnesses, delaying life-saving care. Families should be alert to subtle changes and communicate concerns immediately.
Stage 2: Sepsis with Organ Dysfunction
If early sepsis is not promptly treated, it can progress to sepsis with clear organ dysfunction, previously referred to as “severe sepsis.” This stage may involve:
- Dangerously low urine output
- Shortness of breath
- Altered mental state
- Abdominal pain
- Abnormal heartbeat
Lab results may also show abnormal clotting, elevated liver enzymes, or high lactate levels.
Treatment at this stage typically requires ICU care, intravenous fluids, targeted antibiotics, and interventions to support failing organs, such as dialysis or mechanical ventilation. The medical standard of care demands urgent escalation of treatment, frequent monitoring, and full documentation. Failure in any of these areas can point to negligence, which a skilled medical malpractice lawyer can investigate and use to hold the responsible providers accountable.
Stage 3: Septic Shock - The Most Life-Threatening Stage
Septic shock is the most critical form of sepsis, defined by the Sepsis-3 consensus as sepsis with persistent low blood pressure requiring vasopressor medications and serum lactate levels greater than 2 mmol/L despite adequate fluid resuscitation. Mortality rates for this stage remain alarmingly high, with sepsis accounting for 19.7% of deaths worldwide.
At this stage, patients require immediate intensive care with vasopressors to stabilize blood pressure, mechanical ventilation for breathing support, and continuous monitoring of every organ system. Even with optimal care, survivors may face long-term complications such as chronic fatigue, cognitive decline, and organ damage.
The Importance of Rapid Medical Response
The Surviving Sepsis campaign guidelines emphasize the one-hour bundle for suspected sepsis cases, meaning patients should receive antibiotics, intravenous fluids, and diagnostic testing within the first hour of recognition. In emergency departments, hospitals, and nursing homes, providers have a duty to recognize the early signs of sepsis and act immediately. This includes ordering critical lab tests, starting broad-spectrum antibiotics, and closely monitoring vital signs.
For families, especially those with loved ones in long-term care, knowing these standards can help identify when proper care may not have been given. If a loved one’s sepsis worsened due to slow or inadequate treatment, a nursing home abuse lawyer at Olson Personal Injury Lawyers can help investigate whether the facility or hospital failed in its responsibilities.
Sepsis in Different Healthcare Settings
Sepsis can develop in any care setting, but the risks vary. Hospitals generally have advanced diagnostics and ICU access, yet overcrowded ERs or high patient loads can delay recognition. In nursing homes, residents are more vulnerable due to age, chronic illness, and limited mobility, but symptoms like confusion or rapid breathing may be dismissed as part of existing conditions. Rehabilitation facilities often have fewer resources, creating inconsistent monitoring.
Care transitions, such as moving from a hospital to a nursing home, are especially risky. These handoffs require clear documentation of symptoms, test results, and care instructions. When facilities fail to communicate or record critical details, diagnosis and treatment can be delayed, allowing sepsis to progress rapidly.
Health Care Challenges in Colorado, New Mexico, and Wyoming
In the Western states, many communities rely on rural health care facilities that face unique challenges in preventing and treating sepsis. Smaller hospitals and nursing homes often operate with limited staff, meaning fewer eyes to monitor patients for early signs of infection. These facilities may lack on-site specialists or advanced diagnostic equipment, forcing providers to make critical decisions with fewer resources.
Distance is another vital factor. In rural Colorado, New Mexico, and Wyoming, emergency transfers to larger hospitals can take hours. Telemedicine has become a valuable tool for connecting smaller facilities with sepsis specialists, but its effectiveness depends on timely use and reliable communication between providers.
When Healthcare Facilities Fall Short: Understanding Your Legal Options
Sepsis-related negligence can occur in any setting, often due to missed warning signs, slow lab results, or poor coordination during facility transfers. When infection history, vital signs, or test results aren’t clearly documented, treatment delays become more likely.
Inadequate staff training and weak communication can also cause early symptoms to be overlooked, allowing a treatable infection to become life-threatening. Families can play a vital role by staying engaged, asking questions, and ensuring care plans are clearly understood across every facility involved.
When these failures result in delayed diagnosis, poor monitoring, or tragic loss, families may need to explore their legal options. This includes understanding medical malpractice vs. negligence, both of which may apply in sepsis cases.
Moving Forward After Sepsis: Recovery and Legal Options
Recovery from sepsis can bring lasting challenges, including fatigue, organ damage, cognitive changes, and post-sepsis syndrome, which can require long-term care and rehabilitation. These burdens affect both survivors and their families.
If delayed diagnosis, poor monitoring, or other preventable errors worsened the condition, a legal consultation may help. Olson Personal Injury Lawyers has extensive experience with medical malpractice cases involving sepsis in hospitals, nursing homes, and rehab facilities. Our zero-fee guarantee means you pay nothing unless we win, and our 30-day guarantee allows you to try before you commit, ensuring you’re satisfied with the help you receive. During your consultation, we’ll review the care provided, explain your options, and connect you with resources for ongoing support.
Conclusion: Knowledge and Advocacy Save Lives
Sepsis can become life-threatening in hours, making early recognition and prompt treatment essential. Families who ask questions, push for timely care, and stay alert to changes can help prevent tragedy.
If you suspect negligence contributed to a sepsis-related injury or loss, our team at Olson Personal Injury Lawyers has a track record of securing life-changing case results and is ready to help.
Call (303) 381-2234 or contact us online for a free consultation and learn how we protect the West, one case at a time.